Plantar warts are a type of skin growth caused by the human papillomavirus (HPV). They typically appear on the soles of the feet, hence the name "plantar" warts. These warts are characterized by their rough, grainy texture and can often have small black dots in the center, which are clotted blood vessels. While they are usually not a serious medical concern, they can be painful, especially when they develop on weight-bearing areas of the foot.
Plantar warts are highly contagious, and they can be contracted through direct or indirect contact with the virus. Common ways in which they can be transmitted include: * Walking barefoot in public places such as locker rooms, swimming pools, and communal showers. * Sharing towels, socks, or shoes with someone who has plantar warts. * Scratching or picking at an existing wart, which can spread the virus to other parts of your foot. Several factors can increase your risk of developing plantar warts: * Weakened Immune System: People with weakened immune systems, such as those with autoimmune disorders or on immunosuppressive medications, are more susceptible to plantar warts. * Frequent Foot Moisture: Prolonged exposure to moist environments can make the skin more susceptible to the virus. * Skin Abrasions: Open cuts or skin abrasions on the soles of the feet provide an entry point for the virus. Symptoms The symptoms of plantar warts can vary, but common signs to look out for include: * A small, fleshy growth on the bottom of the foot. * Rough, grainy texture on the surface. * Pain or tenderness when walking or standing, especially if the wart is located on a pressure point. * Black dots (clotted blood vessels) within the wart.
Plantar warts can be stubborn and may not go away on their own. At Adler Podiatry, we offer a range of effective treatment options to address this condition: * Topical Medications: Over-the-counter wart treatments containing salicylic acid can be effective in gradually wearing down the wart. Our podiatrists can recommend the right products and provide guidance on their use. * Cryotherapy: Cryotherapy involves freezing the wart with liquid nitrogen to destroy the affected tissue. This is typically done in a clinical setting. * Prescription Medications: In some cases, your podiatrist may prescribe stronger medications or topical treatments to address the wart. * Surgical Removal: For stubborn or painful warts, surgical removal may be necessary. This can include excision, laser therapy, or electrocautery.
Prevention is always the best strategy when it comes to plantar warts. Here are some steps you can take to reduce your risk of contracting or spreading the virus: * Avoid walking barefoot in public places and wear flip-flops or shower shoes in communal areas. * Keep your feet clean and dry. Dry feet are less likely to develop warts. * Don't share towels, socks, or shoes with someone who has plantar warts. * Avoid picking or scratching at existing warts, as this can spread the virus to other areas of your foot.
Plantar warts can be a nuisance, but with the right knowledge and expert care from Adler Podiatry, you can effectively manage and treat this common foot condition. If you suspect you have plantar warts or are experiencing discomfort in your feet, don't hesitate to seek professional help. Our skilled podiatrists are here to provide you with the guidance and treatment you need to get back on your feet comfortably and confidently.


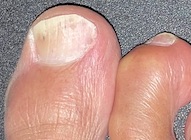 Topical chemicals and medications i.e. alcohol, Vicks VapoRub,® Lamisil Cream® and Tinactin Powder® are able to suppress fungal growth.
Topical chemicals and medications i.e. alcohol, Vicks VapoRub,® Lamisil Cream® and Tinactin Powder® are able to suppress fungal growth.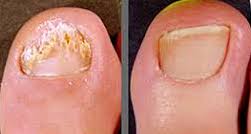 Non-prescription antifungals may not penetrate the toenail or may damage the cells of the nailbed. Topical prescription medication i.e. Ciclopirox® and Jublia® may penetrate the toenail, but may not completely kill the fungus.
Non-prescription antifungals may not penetrate the toenail or may damage the cells of the nailbed. Topical prescription medication i.e. Ciclopirox® and Jublia® may penetrate the toenail, but may not completely kill the fungus.